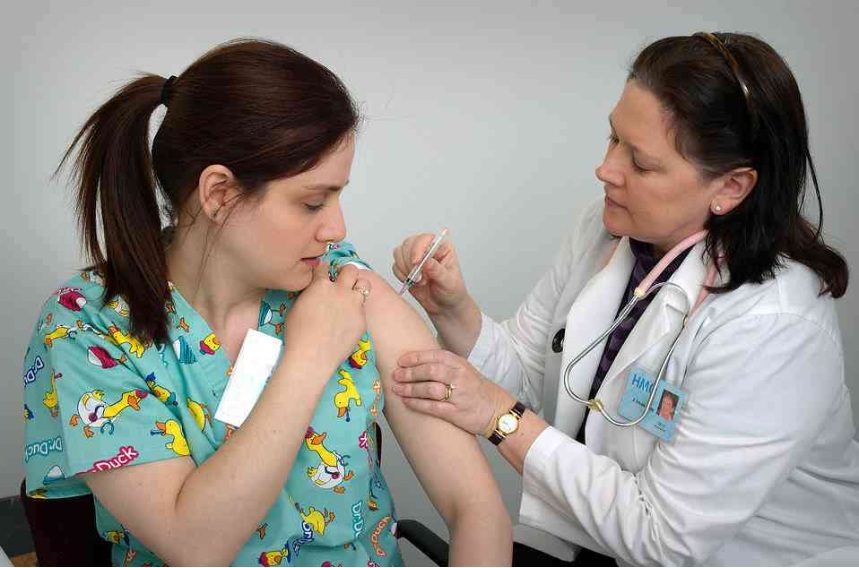
Are Autoimmune Diseases Inherited and Can You Lower Your Risk?
Genetics of Autoimmune Diseases: Are You Doomed Just Because of Your Genes?
There are a lot of misconceptions surrounding genetics and autoimmune diseases. When someone is diagnosed with a condition like lupus, rheumatoid arthritis, Hashimoto’s, or even type 1 diabetes, doctors—especially in conventional medicine—often say, “It’s just genetics.” This leads many people to think, “It’s my genetics, there’s nothing I can do about it.” But does having a genetic risk for an autoimmune disease really mean you’re guaranteed to develop one?
Here’s the good news: Just because you have a genetic predisposition to autoimmune diseases doesn’t mean you’re destined to get one. While you can’t change your genetics, you can control aspects of your lifestyle, diet, and environment.
As the saying goes, “Genetics load the gun, but lifestyle pulls the trigger.” The key is to address lifestyle, dietary, and environmental factors that act as the trigger for autoimmune conditions.
In this post, I’ll dive into the genetics of autoimmune diseases, the genes involved, and what steps you can take to reduce your risk or manage the condition if you’re already affected.
How Do Genes and Gene Mutations Affect My Health?
DNA, or deoxyribonucleic acid, serves as your genetic blueprint, coding for every cell, protein, and molecule in your body. When base pairs in this genetic code are altered, mutations can occur, potentially changing how proteins or cells function. Genes can also be turned on or off, influencing your health in either a positive or negative way. This is where epigenetics comes into play. Remember, just because you have a certain gene doesn’t necessarily mean it will cause problems. Now, let’s explore some autoimmune conditions and how genetics plays a role in them.
Is Rheumatoid Arthritis a Genetic Disease?
There’s no single “autoimmune gene,” but some autoimmune diseases are linked to specific genetic variations. For rheumatoid arthritis, certain genes can slightly increase your risk, particularly when combined with environmental triggers. Key genes associated with rheumatoid arthritis include:
- STAT4: This gene activates the immune system and plays a role in other autoimmune conditions like lupus.
- TRAF1/C5: This gene is linked to chronic inflammation.
- PTPN22: It regulates immune cell responses and is one of the most commonly implicated genes in RA.
Another gene often associated with rheumatoid arthritis is HLA-DR4 (human leukocyte antigen). People with this gene variation are more likely to develop RA compared to those without it. Additionally, genetic markers can help predict how well a person will respond to treatment.
Genetics and Lupus
If you’ve wondered if lupus is hereditary, research shows that some gene variations are associated with systemic lupus erythematosus, a condition that tends to run in families. While having a family member with lupus does increase your risk, most cases are sporadic. Around 30 different genes have been linked to lupus, and people of African, Asian, Pacific Island, Hispanic/Latino, Native American, or Native Hawaiian descent have a higher genetic risk for the condition.
Is Crohn’s Disease Inherited?
Many people ask if Crohn’s disease is genetic. Studies have found over 200 genetic variations linked to Crohn’s disease, particularly those involved in immune system function. These genes include:
- ATG16L1
- NOD2
- IL23R
- IRGM
These genes help the immune system respond properly to bacteria in the intestinal lining. When mutated, they can cause the immune system to overreact, leading to inflammation and digestive issues associated with Crohn’s.
Is Ulcerative Colitis Genetic?
Ulcerative colitis (UC) also has a genetic component. People with certain gene variations, especially those with a family history of UC, are more likely to develop the condition. More than 70 genes are thought to increase the risk of inflammatory bowel diseases like UC. Many of these genes also relate to other autoimmune diseases like psoriasis.
Genes related to UC often affect the proteins that form the protective barrier of the intestines. When this barrier is compromised, harmful bacteria and toxins can enter the bloodstream, triggering an immune response.
Are You Doomed to Get an Autoimmune Disease?
Here’s the good news: Knowing your genetic risks allows you to take preventative action. You can make lifestyle changes to minimize environmental triggers. Even if you have poor genetic markers, staying on top of your diet and lifestyle can help keep your body functioning well and reduce the likelihood of developing autoimmune diseases.
Often, what seems like a genetic problem may actually be tied to shared lifestyle factors in your family. For example, autoimmune diseases like lupus and Hashimoto’s tend to run in families, but it may not just be their genes they have in common—it could also be their environment, diet, and lifestyle.
Understanding your triggers is essential. Stress management, for instance, can be a key factor in preventing autoimmune issues. The goal is to recognize all potential triggers and use this knowledge to prevent the disease from developing or progressing.
The Gut Microbiome and Genetics
The gut microbiome, made up of bacteria and microorganisms in the intestines, can also influence your genes and autoimmunity. The microbes in our microbiome outnumber human cells, so they have a significant impact on our genetics.
Gene-Environment Interaction: Epigenetics
Your environment can trigger gene variations that contribute to autoimmune diseases. Environmental factors like toxins, chemicals, diet, stress, and infections can lead to changes in gene expression. These changes, known as epigenetic changes, don’t alter your genetic code but can influence how your genes function.
Epigenetics can increase vulnerability to diseases, including autoimmune conditions. Factors like exposure to toxins, stress, nutrient deficiencies, and other lifestyle elements can lead to these changes. They often affect the microbiome, which can have long-lasting health effects.
Epigenetic changes don’t just affect you; they can also impact future generations. One type of epigenetic change, DNA methylation, acts as a switch that can turn genes on or off.
Nutrigenomics and Genetics
Nutrigenomics is the study of how diet affects gene expression. Your nutrient levels, or lack thereof, can influence which genes are activated. For example, during the 1944-45 famine in the Netherlands, pregnant women suffered from severe nutrient deficiencies. Studies later showed that children born during this time were more prone to conditions like schizophrenia, stress sensitivity, and obesity, illustrating how nutrition can impact genetic susceptibility to diseases.